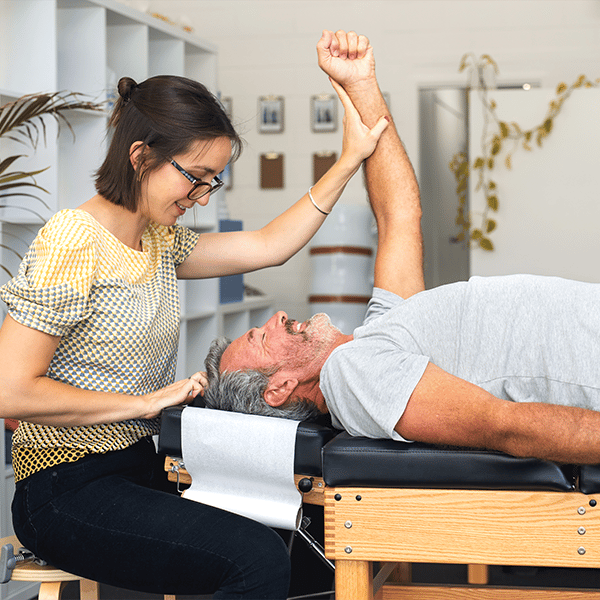
This October during National Chiropractic Health Month, the American Chiropractic Association and doctors of chiropractic nationwide are working together to promote better access to non-drug therapies and remind people that chiropractic’s non-drug approach is on the frontline for pain management, offering evidence-based treatments that are safe and effective and that may help some patients to reduce or eliminate their dependence on prescription opioids. On the Healthy Living blog this month, we are sharing the stories of chiropractors who are “On the Frontline for Pain.”

Aric Frisina-Deyo, DC, MS, is a resident in the neuromusculoskeletal program at the University of Bridgeport. Through the residency program, he provides chiropractic services to Federally Qualified Health Centers in Connecticut. He was also previously an assistant adjunct professor of clinical sciences in the University of Bridgeport School of Chiropractic.
Q: What does a “day in the life” look like in your job?
A: A day in the life starts with getting to the community health center before my first patient at 8 a.m. I take time to review past medical records, primary care office visits, specialist notes and emergency department reports for all my new patients for the day and prep the room for my first visit. If needed, I can send an instant message to the patient’s primary care provider to clarify the reason for referral or any other pertinent questions I might have related to their medical history. I evaluate and treat patients for eight hours a day, with time to coordinate with other on-site providers including primary care, urgent care, dental, podiatry, dieticians and behavioral health as needed through [electronic health records], instant message or in person between patients. Otherwise, I provide high-quality patient-centered care and try to log my notes in a timely manner like any other ACA chiropractor.
Q: Why did you want to become a chiropractor, and how did you end up working in community health centers?
A: I have had chronic low back pain since my early teens. I had run the gamut of medical referrals and procedures—physical therapy, NSAIDs (non-steroidal anti-inflammatory drugs), opioids, radiofrequency ablation—without ever really finding significant or lasting relief. Chiropractic care was a tool in my recovery that I did not find until working on my Master of Health Education degree. I could not downplay the benefit I had with [chiropractic care]—it allowed me to move and feel better than I had in years. I set out to find and shadow a chiropractor who took a patient-centered approach including exercise prescription, nutritional counseling and manual therapy techniques. Next, I set out to find an educational program which relied on the available evidence in its curriculum and was partnered closely with multi-disciplinary organizations like the VA or Community Health Centers Inc. Following graduation at the University of Bridgeport School of Chiropractic, I accepted a residency position and began providing care at community health centers across the state of Connecticut while also pursuing a Diplomate of the International Academy of Neuromusculoskeletal Medicine (DIANM) certification.
Q: What type of injuries or pain do your patients experience?
A: Primarily chronic pain syndromes and high-impact chronic pain—often due to repetitive manual labor jobs or following traumatic injuries. I see very few patients presenting with acute neuromusculoskeletal (NMSK) conditions. Speaking generally, the painful conditions I encounter most include those common to a majority of chiropractic practices such as low back pain with and without radiculopathy (pinched nerve), neck pain with and without radiculopathy, hip, shoulder and knee pain. Some of the things that appear to set apart the patients seen within these community health centers are the numerous co-morbidities and frequency with which the patients have co-occurring neurologic or rheumatologic diagnoses, have disabilities/life activity limitations due to their painful condition (creating the distinction of high-impact chronic pain), have severe co-occurring mental health conditions and/or are dealing with poverty and homelessness—all of which can be complicating factors in a patient’s recovery from an injury or painful condition.
Q: How do chiropractors help patients at community health centers?
A: Chiropractors at community health centers employ a number of techniques to aid in patient recovery, including spinal and extremity manipulation, manual therapy and soft tissue technique application, and rehab exercise prescription. Additionally, proper patient education and peer-to-peer provider care coordination/guidance for primary care providers during and following a trial of chiropractic care can lead to greater efficiency in care pathways.
Medical providers and other allied health professionals are often overburdened and overworked. NMSK conditions are not always the chief concern when presented with a patient dealing with mental health disorders and multiple chronic physical health conditions, all while attempting to overcome severe health disparities and socioeconomic factors. This is where chiropractic providers shine in community health centers—not only by reducing burden for these other providers, but by affecting a change in these patients whose lives and other medical conditions will be much better managed if their pain is reduced, exercise capacity increased, and they are given some hope about the future of their painful NMSK condition(s).
Q: What makes the chiropractic approach different?
A: Speaking of my experience only, the chiropractic approach to treating NMSK pain is more goal driven, personal and patient centered. Rather than treating disorder “X” with treatment “Y,” we often have the time to build human connection and get to know our patients, build a goal-driven treatment plan which goes beyond treating disorder “X,” and affect a patient’s quality of life by managing painful conditions that go beyond the pain itself.
Q: Why is it important for the public/your patients to have access to non-drug pain management options?
A: The Chiropractic Neuromusculoskeletal Medicine Residency was born on the back of the opioid epidemic and a Federally Qualified Health Center (FQHC) looking for alternative care pathways for patients that were suffering as a result of prior over-prescription. Years later, while the opioid over-prescription crisis has been more controlled, there are still greater than an estimated 2 million individuals with an opioid-use disorder. As chiropractic providers well versed in the pain science behind chronic pain, central sensitization and opioid-induced hyperalgesia, we are uniquely positioned to help those patients whose drug use was in some way related to a NMSK condition. Furthermore, FQHCs are the healthcare point of contact for many underprivileged and underserved populations, many of whom have little knowledge of the chiropractic profession nor have the financial means to access our care. These populations are disproportionately affected by disability related to NMSK conditions and often come to us with varied and complex medical histories/problems that need co-management. Having access to non-drug pain management is of the utmost importance for these individuals for reasons that may be clinically indicated, personal or financial.
Q: What does it mean to you to be “on the frontline for pain”?
A: To be “on the frontline for pain” means that I am actively engaged in caring for patients dealing with pain. Treatment, whether it be education, adjustments, soft tissue techniques or exercise prescription, all function to help each patient understand, control and overcome their pain and prepare for a brighter tomorrow.
Q: What is one thing that the public should know about chiropractic?
A: Chiropractic is a profession, not a treatment or technique. We provide holistic non-drug treatments primarily focusing on NMSK diseases and disorders utilizing a patient-centered approach. This allows for increased focus on the individual that is suffering from a condition, rather than the condition and its symptoms that just happen to be attached to an individual.